Spinal Deformities
Scoliosis-Congenital and Childhood
Scoliosis is abnormal side-to-side curvature of the spine. The spinal curve may develop as a single curve (shaped like the letter C) or as two curves (shaped like the letter S). In children and teens, scoliosis often does not have any noticeable symptoms and may not be noticeable until it has progressed significantly. The two most common forms are degenerative scoliosis and idiopathic scoliosis (adolescent). Three orthopedically approved options exist for combating scoliosis: observation, bracing, or surgery.
Types of idiopathic scoliosis are categorized by both age at which the curve is detected and by the type and location of the curve. When grouped by age, scoliosis usually is categorized into three age groups:
- Infantile scoliosis: from birth to 3 years old
- Juvenile scoliosis: from 3 to 9 years old
- Adolescent scoliosis: from 10 to 18 years old.This last category of scoliosis, adolescent scoliosis, occurs in children age 10 to 18 years old, and comprises approximately 80% of all cases of idiopathic scoliosis. This age range is when rapid growth typically occurs, which is why the detection of a curve at this stage should be monitored closely for progression as the child’s skeleton develops.
- Terms that describes the location of the curve: Thoracic scoliosis is curvature in the middle (thoracic) part of the spine. This is the most common location for spinal curvature.
- Lumbar scoliosis is curvature in the lower (lumbar) portion of the spine.
- Thoracolumbar scoliosis is curvature that includes vertebrae in both the lower thoracic portion and the upper lumbar portion of the spine.
- Scoliosis curves are often described based on the direction and location of the curve. Physicians have several detailed systems to classify specific curves.
- The most commonly known type of scoliosis is idiopathic scoliosis.
- Other types of scoliosis include: Congenital scoliosis, which develops in utero and is present in infancy. A rare condition, affecting one in 10,000, there is no known cause, but in most cases the spinal curve must be corrected surgically.
- Neuromuscular scoliosis, which sometimes develops in individuals who cannot walk due to a neuromuscular condition such as muscular dystrophy or cerebral palsy. This may also be called myopathic scoliosis.
- Degenerative scoliosis (adult scoliosis), which is a common condition that occurs later in life as the joints in the spine degenerate.
- Rarely, scoliosis is caused by spinal lesion or tumor. Patients who are usually younger (age 8 to 11) than typical scoliosis patients will experience symptoms such as pain, numbness and a left-curving thoracic spine (levoscoliosis). A physician who sees any or a combination of these symptoms will order additional diagnostic tests, such as an MRI, to rule out the possibility of spinal tumor or other lesions as a cause of scoliosis.
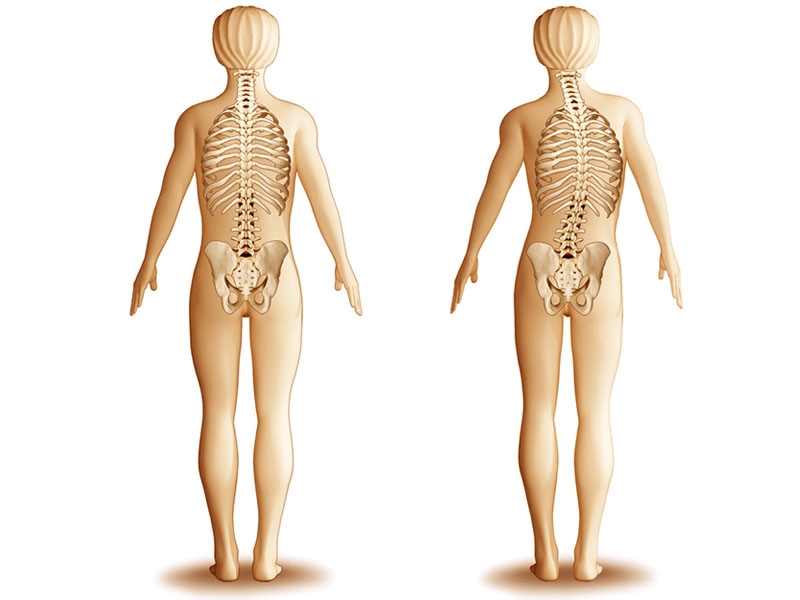
- In children and teenagers, scoliosis often does not have any noticeable symptoms. The curvature of the spine does not cause pain, and if it is mild, it can go unnoticed.While a healthy spine, when viewed from the side, has natural curvature, when viewed from the back the spine appears as a straight line. A person with scoliosis, however, will appear to have a lateral (side-to-side) curve in their spine when viewed from the back.
Signs of Scoliosis
Without an X-ray of the spine, there are several common physical symptoms that may indicate scoliosis. One of the most common tests for detecting scoliosis is called the Adam's Forward Bend Test, in which the individual bends from the waist as if touching the toes. The medical professional then observes for one or more of the following signs of scoliosis:
- One shoulder is higher than the other
- One shoulder blade sticks out more than the other
- One side of the rib cage appears higher than the other
- One hip appears higher or more prominent than the other
- The waist appears uneven
- The body tilts to one side
- One leg may appear shorter than the other
- Any type of back pain is not usually considered a scoliosis symptom.
The risk of curvature progression increases during puberty when the growth rate of the body is the fastest. Scoliosis with significant curvature of the spine is much more prevalent in girls than in boys, and girls are eight times more likely to need treatment for scoliosis because they tend to have curves that have a greater probability of progression. Still, the majority of all cases of scoliosis are mild and do not require treatment.
Pain Needs Further Investigation
Pain is not a typical symptom of scoliosis. Back pain in a child or teen who has scoliosis may indicate another problem and the child should be evaluated by a pediatrician and/or spine specialist. If a child or teen has back pain and also has scoliosis, it is very important
that he or she see a doctor to find out the cause of the pain, as it is probably something other than the scoliosis causing the back pain and may require treatment.
Neurologic Pain and Numbness
Pain and/or leg numbness that signals a neurologic injury is also a very rare presenting symptom of scoliosis. In this case, spinal curvature is caused by a spinal lesion or tumor. Signs that scoliosis is caused by an injury to the spine are:
- Patient is slightly younger (8-11) than a typical scoliosis patient
- Patient is experiencing pain and numbness that indicates a neural impingement
- Thoracic or thorocolumbar curve that leans to the left (levoscoliosis)
- A patient with any or a combination of the above symptoms should receive diagnostic tests, such as an MRI, to discover whether there is a neurologic injury present; if so, immediate treatment is typically recommended.
- Early detection is essential for scoliosis treatment to be most effective. In general, people with a family history of spinal deformity are at greater risk for developing idiopathic scoliosis.
Early Detection for Scoliosis
Frequently, a scoliosis curve in the spine is first diagnosed in school exams or during a regular checkup with a pediatrician. Most students are given the Adam's Forward Bend Test routinely in school when they are in fifth and/or sixth grade to determine whether or not they may have scoliosis. The test involves the student bending forward with arms stretched downward toward the floor and knees straight, while being observed by a healthcare professional. This angle most clearly shows any scoliosis symptoms which present as asymmetry in the spine and/or trunk of the adolescent's body.
Further Scoliosis Testing
Because a scoliosis curvature is usually in the thoracic or thoracolumbar spine (upper back or mid back), if a rib hump or asymmetry of the lumbar spine is found, or
if the shoulders are different heights, it is possible that the individual has scoliosis. If this is the case, follow-up with a physician for a clinical evaluation and an X-ray is the next step.
Physician's exam: The clinical evaluation with the physician will usually include a physical exam, during which the physician will also test to make sure that there are no neurological deficits. Neurological deficits due to scoliosis are uncommon but necessary to check for because there are rare causes of scoliosis that may have spinal cord involvement. X-ray: The X-ray is ordered to both confirm the scoliosis diagnosis and check on the magnitude of the spinal curvature. The X-ray will also give some indication as to the skeletal maturity of the patient which may influence treatment decisions. In rare instances a physician also may request an MRI scan of the thoracic and/or cervical spine to explore the possibility of an intracanal spinal lesion. Signs of a spinal lesion include:
Neurological deficits, such as leg numbness or weakness, that indicate impingement of the spinal cord (e.g. brisk reflex) A left-sided thoracic curvature, called levoscoliosis (the curves are almost always right sided) If the child is younger (e.g. 8-11 years old) than a typical patient with scoliosis.
Formulating a Treatment Plan
Depending on the results of the physician's clinical evaluation and the diagnostic tests, a scoliosis treatment plan will be recommended that may include observation, bracing, or possibly surgery to reduce or correct the spinal curve.
Scoliosis treatment decisions are primarily based on two factors: The skeletal maturity of the patient (or rather, how much more growth can be expected) The degree of spinal curvature.
Although the cause of idiopathic scoliosis is unknown, the way scoliosis curves behave is well understood. In essence: A small degree of curvature in a patient nearing skeletal maturity is not likely to need
treatment; Conversely, a younger patient with a bigger curve is likely to have a curve will continue to advance and will need treatment. There are three main scoliosis treatment options for adolescents:
- Observation
- Back braces
- Scoliosis surgery
No exercises for scoliosis have proved to reduce or prevent curvature. However, exercise is highly recommended for both scoliosis and non-scoliosis patients alike to keep back muscles strong and flexible.
Conservative Treatment Options for Scoliosis
Observation
Once scoliosis is detected, observation by a physician is the next step. The physician will measure the curve on a regular schedule and base treatment decisions on the rate of curvature progression.
Measuring and Tracking Scoliosis Curves
The orthopedic surgeon may order an X-ray of the spine and use the "Cobb method" - an extremely accurate measuring technique - to calculate the curvature of the spine and its progression. Curves that are less than 10 degrees are not considered to represent scoliosis but are considered to be spinal asymmetry. These types of curves are extremely unlikely to progress and generally do not need any treatment, but the child's physician should continue to monitor the curve during regular checkups. Curves beyond 20 to 30 degrees in a growing child should be observed at 4 to 6 month intervals by an orthopedic surgeon with expertise in scoliosis. In a patient that is still growing, treatment will be needed if the following factors are present: The spinal curve progresses more than 5 degrees during a typical period of observation, or; the spinal curve has already reached 30 degrees or more. If the curve progresses less than 5 degrees during a specified period of observation, the physician may determine that the curve is not worsening rapidly enough to cause deformity, and treatment may not be necessary.
Brace Treatment For Scoliosis
Back Braces for Scoliosis
Scoliosis treatment for patients with progressing curves, or curves over 25 degrees in a skeletally immature patient (e.g. girls who are about 11 to 13 years old, and boys who are about 12 to 14 years) is usually centered on use of a back brace. Bracing typically is not used for adolescents who are already skeletally mature or almost mature. If an older child has a curve greater than 30 degrees and is almost mature, his or her curvature will be treated with observation only, as there is little growth left and bracing will unlikely do much good. Bracing does not straighten the curve that is already present. Instead, the goal of a back brace is to stop the progression of the spinal curve as the child continues to grow. The child will continue to wear the brace until he or she reaches skeletal maturity. Once the individual stops growing, there is little likelihood of progression of a curve. Curves that are greater than 50 degrees in angulation can continue to progress after skeletal maturity, so the treatment objective of a back brace is to try to get the child into adulthood with less than a 50-degree curvature.
Fitting and Wearing a Back Brace
Working under the direction of an orthopedic surgeon, an orthotist will fit a custom brace to the individual. The braces usually are made of molded plastic and fit tightly around the body and are worn under the clothes every day. Some are worn overnight; some are worn 23 hours a day.
Although braces for scoliosis are more comfortable than ever before, they still have a low compliance rate for various reasons: children and adolescents feel different from their peers when they have to wear them, and some genuinely cause discomfort and perhaps difficulty breathing. Support for children wearing back braces is key to their effectiveness. Studies clearly show that the more closely patients follow their prescribed bracing regimen, the less the scoliosis curve progresses.
Two Main Types of Back Braces
There are two types of commonly used scoliosis braces (There are many other brace types including rigid and semirigid types but no evidence of superiority of one over the others): The TLSO (thoracolumbar sacral orthosis), which includes a popular model called the Boston Brace, is a custom-molded back brace that applies three-point pressure to the curvature to prevent its progression. It can be worn under loose fitting clothing, and is usually worn 23 hours a day. This type of scoliosis brace can be taken off to swim or to play sports. A Charleston bending back brace applies more pressure and bends the child against the curve. This type of scoliosis brace is worn only at night while the child is asleep. Unfortunately, even with appropriate bracing, some scoliosis spinal curves will continue to progress. For these cases, especially if the child is very young, bracing may still be continued to allow the child to grow before fusing the spine.
Surgical Treatment in Scoliosis
Surgery for adolescents with scoliosis is only recommended when their curves are greater than 40 to 45 degrees and continuing to progress, and for most patients with curves that are greater than 50 degrees. Unlike back braces, which do not correct spinal curves already present, surgery can correct curvature by about 50%. Furthermore, surgery prevents further progression of the curve. There are several approaches to scoliosis surgery, but all use modern instrumentation systems in which hooks and screws are applied to the spine to anchor long rods. The rods are then used to reduce and hold the spine while bone that is added fuses together with existing bone. Once the bone fuses, the spine does not move and the curve cannot progress. The rods are used as a temporary splint to hold the spine in place while the bone fuses together, and after the spine is fused, the bone (not the rods) holds the spine in place. However, the rods are generally not removed since this is a large surgery and it is not necessary to remove them. Occasionally a rod can irritate the soft tissue around the spine, and if this happens, the rod can be removed.
Two Approaches to Scoliosis Surgery
There are two general approaches to the scoliosis surgery - a posterior approach (from the back of the spine) and an anterior approach (from the front of the spine). Specific surgery is recommended based on the type and location of the curve. Recently, the number of anterior approaches have diminished significantly as our ability to perform the whole surgery from posterior has increased.
Surgical Treatment In Scoliosis-Continued
1. Scoliosis Surgery from the Back (Posterior Surgical Approach)
This approach to scoliosis surgery is done through a long incision on the back of the spine (the incision goes the entire length of the thoracic spine). The muscles are retracted to the sides to expose the spine. The spine is then instrumented (screws are inserted) and the rods are used to reduce the amount of the curvature. Bone is then added (either the patient's own bone, taken from the patient's hip, or cadaver bone), inciting a reaction in which the bones in the spine begin fusing together. The bones continue to fuse after surgery is completed. The fusion process usually takes about 3 to 6 months, and can continue for up to 12 months. For patients who have a severe deformity and/or those who have a very rigid curvature, another procedure may be required prior to this surgery. A surgeon may recommend an anterior release of the disc space (removal of the disc from the front), which involves approaching the front of the spine either through an open incision or with a scope (thoracoscopic technique) and releasing the disc space. After the discs at the appropriate levels of the spine have been removed, bone (either the patient's own bone and/or cadaver bone) is added to the disc space to allow it to fuse together. Removing the discs allows for a better reduction of the spine and also results in a better fusion. These two factors are especially important if the patient is a young child (10 to 12 years old) and has a lot of skeletal growth left. Without the anterior release procedure, the anterior column (the part of the spine facing the front of the body) can continue to grow, eventually twisting around the fused, non-growing posterior spinal column, forming a new scoliosis curve (called "crankshafting"). Fusing the spine anteriorly prevents this process.
2. Scoliosis Surgery from the Front (Anterior Surgical Approach)
For curves that are mainly at the thoracolumbar junction (T12-L1), the scoliosis surgery can be done entirely as an anterior approach. This approach to scoliosis surgery requires an open incision and the removal of a rib (usually on the left side). Through this approach, the diaphragm can be released from the chest wall and spine, and excellent exposure can be obtained for the thoracic and lumbar spinal vertebral bodies. The discs are removed to loosen up the spine.Screws are placed in the vertebral bodies and rods are put in place to reduce the curvature. Bone is added to the disc space (either the patient’s own bone, taken from the patient's hip, or cadaver bone), to allow the spine to begin to fuse together. This fusion process usually takes about 3 to 6 months, and can continue for up to 12 months.If this surgery is applicable because of the type of curvature, the anterior approach to scoliosis surgery has several advantages over the posterior approach. Not as many lumbar vertebral bodies will need to be fused and some additional motion segments can be preserved. Saving motion segments is especially important for lower back curves (lumbar spine), because if the fusion goes below L3 there is a higher risk of later back pain and arthritis. Saving lumbar motion segments also helps prevent loading all the stress on just a few motion segments. This approach can sometimes allow for a better reduction of the curve and a more favorable cosmetic result. The major disadvantage of the anterior approach is that it can only be done for thoracolumbar curves, and most scoliotic curves are in the thoracic spine.
Risks of Scoliosis Surgery
1. Paraplegia
The most concerning risk with scoliosis surgery is paraplegia. It is very rare (about 1 in 1,000 to 1 in 10,000 chance) but is a devastating complication. To help manage this risk, the spinal cord can be monitored during surgery through one of two methods: Somatosensory Evoked Potentials (SSEPs). This test involves small electrical impulses that are given in the legs and then read in the brain. If there is the development of slowing of the signals during surgery this can indicate compromise to the spinal cord or its blood supply. Another way to monitor the cord is with Motor Evoked Potentials (MEPs), and often both are used throughout a surgery.
Stagnara wake up test. This test involves waking the patient during the surgery and asking them to move their feet. The patient does not feel any pain during this procedure and will not remember it afterwards.
If either of these tests indicates spinal cord compromise, the rods can be cut out and the surgery abandoned. Fortunately, this situation is extremely uncommon, and many procedures can be rescheduled if the patient is found to be neurologically intact after the surgery.
2. Excessive Blood Loss
Another risk with scoliosis surgery is excessive blood loss. There is a lot of muscle stripping and exposed area during the surgery. With proper technique the blood loss can usually be kept to a reasonable amount and blood transfusions are rarely needed. As a precaution, many surgeons will ask the patient to donate his or her own blood prior to surgery (autologous blood donation), which can then be given back to the patient after the surgery. Also, during scoliosis surgery the patient's blood can be collected and transfused back to the patient.
3. Other Potential Risks and Complications
The rods breaking or the hooks or screws dislodging (although with modern instrumentation systems, this type of hardware failure is quite uncommon)
- Infection (less than 1%)
- Cerebrospinal fluid leak (rare)
- Failure of the spine to fuse (about 1%-5%)
- Continued progression of the curve after surgery
Postoperative Care in Scoliosis Patients
Following scoliosis surgery, patients usually can start to move around about 2 to 3 days after the procedure. The total hospital stay is usually about 4 to 7 days. Patients can return to school about 2 to 4 weeks after surgery, but activity needs to be limited while the bone is fusing.
It is important to note that the more immobile the spine is kept the better it will fuse. Bending, lifting, and twisting are all discouraged for the first three months after surgery. For this reason, some surgeons will prescribe wearing a back brace for a period following the surgery which helps to restrict movement. Any physical contact or jarring type activities are restricted for about 6 to 12 months after surgery.
Generally the patient will be monitored with intermittent examinations and X-rays for 1 to 2 years after the surgery. Once the bone is solidly fused no further treatment is required.
For the most part, patients can resume normal activity levels after a thoracic fusion since fusing the thoracic and upper lumbar spine does not change the biomechanics of the spine all that much. Female patients who have had a scoliosis fusion can still become pregnant and deliver babies vaginally.
Schuermann’s Kyphosis
Scheuermann's disease, or Scheuermann's kyphosis, is a condition in which the normal roundback in the upper spine (called a kyphosis) is increased. Most people with Scheuermann's disease will have an increased roundback (e.g. a hunch back or hump back) but no pain.The name of this condition comes from Scheuermann, the person who in 1921 described changes in the vertebral endplates and disc space that can occur during development and lead to kyphosis, or roundback deformity of the thoracic spine (upper back).
The cause of Scheuermann's disease is unknown, but is thought to be due to a growth abnormality of the vertebral body. The growth plate anteriorly (in the front) stops growing but the posterior part of the growth plate continues to grow. This is due to a condition known as osteochondrosis. The wedge-shape of the vertebra creates an increase in the amount of normal kyphosis (front angulation of the thoracic spine) The wedging of vertebrae in Scheuermann’s kyphosis is most common in the thoracic spine (upper back), with the apex of the curve typically between the T7 and T9 levels of the spine. Although less common, Scheuermann’s kyphosis may also occur in the junction between the thoracic and lumbar spine (thoracolumbar spine) or in the lumbar spine (lower back). Scheuermann’s disease does not spread and is not really a “disease” but a condition that can arise during growth. It is more common in males and appears in adolescents usually towards the end of their growth spurt. If the roundback deformity is severe, patients are more likely to have discomfort or pain along with the deformity as they age.
The normal curvature of the thoracic spine is between 20 and 50 degrees. A curvature of more than 50 degrees, where the spine has three contiguous vertebral bodies that have wedging of 5 degrees or more, constitutes Scheuermann’s disease.Postural roundback in adolescents is most often caused by posture and not by structural changes to the spine. Postural roundback can be easily distinguished from Scheuermann’s kyphosis by the fact that the deformity goes away when the patient lies down. Typically, patients with true Scheuermann’s kyphosis need to sleep on two or three pillows at night to stay comfortable because there deformity remains when they lie down.Most patients with Scheuermann’s also have a mild scoliosis (when the spine curves to the side). These mild scoliosis curves rarely require treatment. As with scoliosis, an X-ray is used to confirm a diagnosis of Scheuermann’s disease.
Treatment Options for Scheuermann's Disease:Treatment of Scheuermann’s disease is indicated to relieve pain, to correct an unacceptable cosmetic deformity, and to prevent potential progression or worsening of the curve. Treatment will vary depending on the size of the curve, the flexibility of the curve, the patient’s age and the patient’s preferences
Conservative Treatments for Scheuermann's Disease: For patients with more than one year of growth left, the kyphosis can be partially reversed by wearing a brace (e.g. a Milwaukee brace). The brace can improve the curve during the growing years by restoring height to the front of the vertebral body and sometimes can reduce pain if present. Depending on the severity and progression of the curve, patients may be prescribed a brace for one to two years.For patients who are already skeletally mature, bracing is not an effective treatment.An exercise program, including specific strengthening and hamstring stretching exercises, may be recommended in conjunction with bracing. While exercise won’t correct the deformity, it can be helpful in alleviating back pain and fatigue.
Surgery for Scheuermann's Disease: Surgery is rarely needed for Scheuermann’s disease. It may be considered for patients with severe deformities (e.g. more than 70 degrees for thoracic kyphosis), if neurological deficits are present, and occasionally if pain is present with the deformity. The goal of the surgery is mostly to reduce the deformity, although some feel it can lessen pain if present. Surgery historically included:A front thoracotomy (approach through the chest) to release the tissues, remove the discs, and place bone graft in the spaces to fuse the thoracic spine, then posterior surgery was done. But today, the spine is approached from the back and instrumentation (such as rods, bars, wires, or screws, which hold the spine straight during the fusion process) is put in place. After surgery, provided the fusion is successful, all of the affected segments will be fused into one continuous bone that will not progress into kyphosis. Because Scheuermann’s disease usually occurs in the thoracic spine, which has almost no motion, a fusion in this area does not affect the normal motion of the spine and typically does not lead to pain later in life. Most of the motion in the spine is in the lumbar spine, and it is usually not necessary to fuse this area. This is important to avoid overstressing the other lumbar spinal segments and causing early breakdown at adjacent levels.
In general, in a skeletally mature patient, Scheuermann’s kyphosis is not progressive. This is different from adolescent scoliosis, which can continue to progress (if the deformity is more than 50 degrees) going into adulthood. For adults with Scheuermann’s kyphosis, the treatment is usually observation, anti-inflammatory drugs or reconstructive surgery, depending on the severity of the symptoms.
Juvenile Disc Disorder
Juvenile disc disorder, or juvenile discogenic disorder, represents a condition where the endplates of the disc spaces are not strong enough to withstand the pressures generated within the disc spaces. This leads to disc herniations into the vertebral bodies (called Schmorl’s nodes) and causes back pain at an early age. This condition is sometimes referred to as Scheuermann’s disease, or Lumbar Scheuermann’s disease, but the preferred medical terminology for this condition is juvenile disc disorder. Juvenile disc disorder is not as common as Scheuermann’s kyphosis and is not associated with deformity of the spine. Patients with juvenile disc disorder usually have lower back pain that is made worse with bending forward and activity, and feels better with rest. This condition is very much like degenerative disc disease in the adult population, but the degeneration starts at a much earlier age, and usually involves most of the discs of the lumbar spine (as opposed to only one or two discs typically involved in degenerative disc disease).
Treatments for Juvenile Disc Disorder
Conservative (non-surgical) treatments for juvenile disc disorder are largely the same as for adult degenerative disc disease, and surgery to fuse a segment is rarely advisable. Conservative treatments may include one or a combination of the following:
- Medications
- Chiropractic or osteopathic manipulations
- Epidural injections
- TENS units
- Physical therapy (exercises, stretching)
It is important to note that adolescents who have back pain due to juvenile disc disorder do not need to have their activities medically restricted. In fact, physical activity is encouraged as it can help keep the back strong and healthy. In general, adolescents who are inactive have a higher rate of back pain as they become deconditioned and weaker. There is no conclusive evidence that activity accelerates the disc degeneration, so adolescents with this diagnosis should be allowed to participate in athletics as their pain allows. A well-balanced exercise program of daily hamstring stretching, strength training, and aerobic conditioning is best. Because the degeneration typically occurs in multiple discs, any attempt to fuse one or more levels of the lumbar spine will place a lot more pressure on the already weakened other levels. Fusing the whole spine leads to only more pain as the spine is basically meant to move, and attempts at fusing the whole lumbar spine are rarely successful in reducing pain. Howeve, surgery to remove a disc herniation that is compressing a nerve is reasonable, as a decompression surgery (e.g. microdiscectomy) can relieve pain but does not change the natural biomechanics of the spine. Vocationally, patients with a lot of back pain and evidence of juvenile disc disorder on their imaging studies should be counseled to not consider a heavy manual labor job. Even though manual labor may not accelerate the degeneration, if they use their back for a living but are prone to bouts of low back pain, then they may have a lot of difficulty performing their jobs satisfactorily. In general, people are able to perform a more sedentary job whether or not low back pain is present.
Rheumatoid Kyphosis-Ankylosing Spondilitis
Ankylosing spondylitis (AS) is a type of arthritis that primarily affects the spine. The disease is characterized by inflammation and resulting stiffness and pain in the joints along the spine. The knee and shoulder joints may also be affected.
With ankylosing spondylitis, the inflammation in the joints of the spine will typically result in parts of the vertebrae and joints in the spine fusing together. As parts of the vertebrae grow (or “fuse”) together, the spine becomes more rigid and inflexible.The fusion takes place as a reaction to inflammation of ligaments or tendons at the site of attachment to bone. The inflammation causes bone to erode at the site of the attachment, and then as the inflammation subsides, the body’s natural healing process causes new bone growths in its place. Because this new bone is stiff, as opposed to the elastic quality of the tissue or ligaments, the normal range of motion of the spine is diminished. Ankylosing spondylitis most commonly is diagnosed in young men between the ages of 15 and 30, although it can affect anyone. Almost everyone with ankylosing spondylitis carries a specific gene called HLA-B27.
When it is difficult to perform daily tasks or to look forweard because of the defomity caused by Ankylosing spondilitis, a surgical treatment to correct the kyphotic deformity is advised.
In this surgery, the spine is approached from the back and after exposure, screws are inserted. Then bone cuts are done to the spine to release the fused structures. A bone wedge (sometimes more then 1) is removed and the wedge is closed to correct the kyphosis. Finally the screws are connected to a properly bent rod to hold the corrected spine in a stable position.
The aftercare of an ankylosing spondilitis patient is generally not different form a standard spinal deformity patient. Ambulation is encouraged the next day after surgery and the patients are generally discharged in a week .
Smoking or the use of a specific groups of drugs like steroids and TNF alpha blockers are strongly discouraged as they interfere with and sometimes totally prevent bone healing.