Spinal Fractures
Compression and Burst Fractures
Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can be the result of bones weakened by osteoporosis.
Most spinal fractures occur in the thoracic (midback) and lumbar spine (lower back) or at the connection of the two (thoracolumbar junction). Treatment depends on the severity of the fracture and whether the patient has other associated injuries.
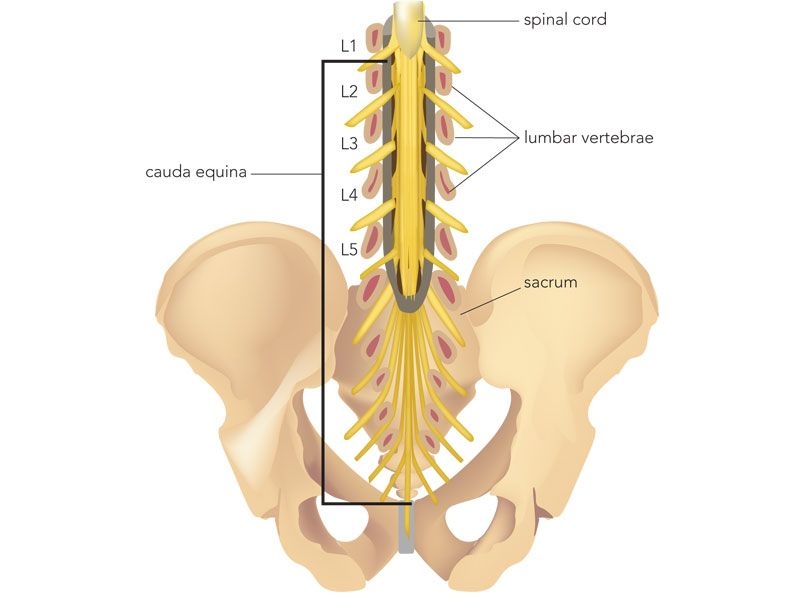
Understanding how your spine works will help you to understand spinal fractures. Learn more about your spine:
Spine Basics
Cause: Fractures of the thoracic and lumbar spine may result from high-energy trauma, such as a:
- Car or motorcycle crash
- Fall from height
- Sports accident
- Violent act, such as a gunshot wound
Many times, these patients have additional serious injuries that require rapid treatment. The spinal cord may also be injured, depending on the severity of the fracture.
Spinal fractures may also be caused by bone insufficiency. For example, people with osteoporosis, tumors, or other underlying conditions that weaken the bone can fracture a vertebra even during low-impact activities--such as reaching or twisting. These fractures may develop unnoticed over a period of time, with no symptoms or discomfort until a bone breaks.
Description: There are different types of spinal fractures. Doctors classify fractures of the thoracic and lumbar spine based upon the specific pattern of the fracture and whether there is a spinal cord injury. Classifying the fracture pattern will help your doctor determine the proper treatment. The three major types of spine fracture patterns are:
Flexion, extension and rotation
Symptoms
A fracture of the thoracic or lumbar spine causes moderate to severe back pain that is worsened with movement.
If the spinal cord is involved, the patient may experience bowel/bladder dysfunction along with numbness, tingling, or weakness in the limbs.
If the fracture is caused by high-energy trauma, the patient may also have a brain injury and lose consciousness, or "black out." There may also be other injuries— called distracting injuries—that cause pain that overwhelms the back pain. In these cases, it has to be assumed that the patient has a fracture of the spine, especially after a high-energy event such as a motor vehicle crash.
Emergency Stabilization
Patients with fractures of the thoracic and lumbar spine that have been caused by trauma need emergency treatment. It may be difficult to assess the extent of their injuries on first evaluation.
At the accident scene, emergency rescue workers will first check the patient's vital signs, including consciousness, ability to breathe, and heart rate. After the vital signs are stabilized, rescue workers will assess obvious bleeding and limb-deforming injuries.
Before moving the patient, the emergency team must immobilize the individual in a cervical (neck) collar and backboard. The trauma team will perform a complete and thorough evaluation in the hospital emergency room.
Physical Examination
The emergency room doctor will conduct a thorough evaluation, beginning with a head-to-toe physical examination of the patient. This will include an inspection of the head, chest, abdomen, pelvis, limbs, and spine.
Tests
Neurological tests. The doctor will also evaluate the patient's neurological status. This includes testing his or her ability to move, feel, and sense the position of all the limbs. In addition, the doctor will test the patient's reflexes to help determine whether there has been an injury to the spinal cord or individual nerves.
Imaging tests. After the physical examination, a radiologic evaluation is required. Depending on the extent of injuries, this may include x-rays, computed tomography (CT) scans, and magnetic resonance imaging (MRI) scans of multiple areas, including the thoracic and lumbar spine
Treatment
Treatment for a fracture of the thoracic or lumbar spine will depend on:
- Other injuries and their treatment
- The particular fracture pattern
Once the trauma team has stabilized all other life-threatening injuries, the doctor will evaluate the spinal fracture pattern and decide whether spine surgery is needed.
Nonsurgical treatment.
Most flexion injuries-including stable burst fractures and osteoporotic compression fractures—can be treated with bracing for 6 to 12 weeks. By gradually increasing physical activity and doing rehabilitation exercises, most patients avoid post-injury problems. Extension fractures that occur only through the vertebral body can typically be treated without surgery. These fractures should be observed closely while the patient wears a brace or cast for 12 weeks.Transverse process fractures are predominantly treated with gradual increase in motion, with or without bracing, based on comfort level.
Surgical treatment. Surgery is typically required for unstable burst fractures that have:
- Significant comminution (multiple bone fragments)
- Severe loss of vertebral body height
- Excessive forward bending or angulation at the injury site
- Significant nerve injury due to parts of the vertebral body or disk pinching the spinal cord
Surgery is usually necessary if there is an injury to the posterior (back) ligaments of the spine. In addition, if the fracture falls through the disks of the spine, surgery should be performed to stabilize the fracture.
Fracture-dislocations of the thoracic and lumbar spine are caused by very high-energy trauma. They can be extremely unstable injuries that often result in serious spinal cord or nerve damage. These injuries require stabilization through surgery. The ideal timing of surgery can often be complicated. Surgery is sometimes delayed because of other serious, life-threatening injuries.
These fractures should be treated surgically with decompression of the spinal canal and stabilization of the fracture. The procedure to decompress the spine is called a laminectomy. In a laminectomy, the doctor removes the bony arch that forms the backside of the spinal canal (lamina), along with any bone or other structures that are pressing on the spinal cord. Laminectomy relieves pressure on the spinal cord by providing extra space for it to drift backward. To perform the laminectomy, your doctor will access your spine with an incision either on your side or on your back. Both approaches allow for safe removal of the structures compressing the spinal cord, while preventing further injury.
Surgical Procedure
The ultimate goals of surgery are to:
- Achieve adequate reduction (return the bones into their proper position)
- Relieve pressure on the spinal cord and nerves
- Allow for early movement
Depending on the fracture pattern, the doctor may perform the procedure through either an anterior (front), lateral (side), or posterior (back) approach—or a combination of all three. There are many types of specialized instruments used in spine surgery. These include metal screws, rods, and cages used to stabilize the spine.
Complications Complications associated with fractures of the thoracic and lumbar spine include:
- Blood clots in the pelvis and legs—these may develop during long periods of bed rest or immobility
- Pulmonary embolism—a blood clot that breaks free and travels to the lungs
- Pneumonia
- Pressure sores
There are also specific complications associated with spinal surgery. These include:
- Bleeding
- Infection
- Spinal fluid leaks
- Instrument failure
- Nonunion
Your doctor will talk with you about these risks and take specific measures to avoid potential complications. These measures may include:
- Early treatment
- Mechanical methods (such as lower leg compression stockings) and medications to protect against blood clots
- Proper surgical technique
- Postoperative programs
Outcomes
Regardless of whether treatment is surgical or nonsurgical, there will be a period of rehabilitation after a fracture has healed. The goals of rehabilitation include:
- Reducing pain
- Restoring mobility
- Returning the patient as closely as possible to his or her preinjury state
Your doctor may recommend both inpatient and outpatient physical therapy to help you achieve these goals. If your fracture was caused by osteoporosis, you are at an increased risk for additional fractures. Your doctor will recommend treatments to address bone density loss during your treatment and recovery. In some cases, there may be issues that delay or complicate rehabilitation and recovery. These issues include inadequate reduction of the fracture, neurologic injury (paralysis), and progressive deformity of the spine.
Pathologic (Osteoporotic) Fractures
As we get older, our bones thin and our bone strength decreases. Osteoporosis is a disease in which bones become very weak and more likely to break. It often develops unnoticed over many years, with no symptoms or discomfort until a bone breaks.
Fractures caused by osteoporosis most often occur in the spine. These spinal fractures — called vertebral compression fractures — occur in nearly 700,000 patients each year. They are almost twice as common as other fractures typically linked to osteoporosis, such as broken hips and wrists.
Not all vertebral compression fractures are due to osteoporosis. But when the disease is involved, a vertebral compression fracture is often a patient’s first sign of a weakened skeleton from osteoporosis.
Why Do The Bones Break?
When the small bones of the spine (vertebrae) weaken from osteoporosis, they can narrow or shrink. This can lead to a rounded back, a hump or a “bent forward” look to the spine. Many people with osteoporosis also note that they are getting shorter over time.
The weakened vertebrae are at a high risk for fracture. A vertebral compression fracture occurs when too much pressure is placed on a weakened vertebra and the front of it cracks and loses height. Vertebral compression fractures are sometimes the result of a fall, although people with osteoporosis can suffer a fracture even when doing everyday things, such as reaching, twisting, coughing, and sneezing.
Symptoms: A vertebral compression fracture causes back pain. The pain typically occurs near the break itself. Vertebral compression fractures most commonly occur near the waistline, as well as slightly above it (mid-chest) or below it (lower back).
The pain often gets worse with standing or sitting for a period of time, and is often relieved by rest or lying down. Although the pain may move to other areas of the body (for example, into the abdomen or down the legs), this is uncommon.
Doctor's Examination
Your appointment will begin with a discussion with your doctor about your symptoms and medical history. While you are standing, your doctor will examine the alignment, or straightness, of your spine and your posture. Your doctor will also push on certain places on your back to try and identify whether your pain is from an injury to the muscle or bones. To make sure there is no injury to the spinal nerve roots, your doctor will conduct a neurologic examination. This includes testing your reflexes and muscle strength.
X-rays
If your doctor suspects a vertebral compression fracture, he or she will order an x-ray image to confirm the diagnosis. Other problems in the spine may also show up on x-rays. Elderly patients with a vertebral compression fracture may also have narrowing of disk space (degenerative disk disease) and/or scoliosis, which is a sideways curve of the spine.
Other Imaging Studies
Other imaging tests may be performed to determine if the vertebral compression fracture is a new (acute) fracture or an older (chronic) fracture.
Magnetic resonance imaging (MRI) scan: This test will show any damage to the soft tissues around the fracture (nerves and disks) in better detail. Because of how it shows bone, it may help your doctor determine how old the fracture is.
Bone scan: A bone scan can pick up a wide range of problems in bone, including fractures. It can also show how old a fracture is.
Computed tomography (CT) scan: Shows soft tissue, as well as bone, and can help your doctor evaluate whether the vertebral compression fracture has extended into the spinal canal, where the spinal cord and nerve roots are located.
Bone Density Testing
When you have a vertebral compression fracture, it is important to assess whether you also have osteoporosis, and, if so, how severe the condition is. X-rays will often show thinning of the bone throughout the spine — a condition known as osteopenia. It is a forerunner to osteoporosis, in which the bone becomes much more fragile. The extent of bone loss can be determined with a bone mineral density scan (DEXA). The results of the DEXA help your doctor estimate your risk for additional fractures in the spine and in other parts of your body. The DEXA results provide important information to help your doctor treat any bone density loss with medications.
Treatment
Nonsurgical Treatment: Most people who suffer a vertebral compression fracture get better within 6 to 8 weeks without specific treatment to repair the fracture. Simple measures, such as a short period of rest and limited use of pain medications, are often all that is prescribed. In some cases, patients are instructed to wear a brace to restrict movement and allow the vertebral compression fracture to heal. If your doctor has also diagnosed osteoporosis, you are at an increased risk for additional vertebral compression fractures and other fractures, such as to the hip and wrist. Your doctor will address treatments for bone density loss during this time.
Surgical Treatment: If you have severe pain that does not respond to initial treatment measures, then surgery may be considered. In the past, the only surgical options available to patients with a vertebral compression fracture involved extensive procedures. Today, vertebral augmentation procedures offer a minimally invasive alternative.
The two types of vertebral augmentation methods available are kyphoplasty and vertebroplasty. The best candidates for these procedures are patients who suffer severe pain from recent vertebral compression fractures. If you are a candidate for vertebroplasty or kyphoplasty, your surgeon will discuss which one may be better for you based on the type of vertebral compression fracture you have.
Kyphoplasty: In a kyphoplasty, a small device called a balloon tamp is inserted into the fractured vertebra. The balloon tamp is inflated from within the vertebra, which restores the height and shape of the vertebral body. When the balloon tamp is removed, it leaves a cavity that is filled with a special bone cement that strengthens the vertebra.. Kyphoplasty can be performed using general anesthesia (which puts you to sleep) or with a local anesthesia (which numbs your body around the fracture). In this procedure, the patient lies face down on the operating table and the surgeon accesses the spine from the back. After surgery, patients can go back to all their normal activities of daily living as soon as possible, with no restrictions.
Vertebroplasty: Vertebroplasty is a technique similar to kyphoplasty, but a balloon tamp is not used to create a space for the cement. Instead, the cement is injected directly into the narrowed vertebra. Like kyphoplasty, this procedure is performed while the patient is lying face down so that the surgeon can access the fractured vertebra from the back. After this surgery, patients are encouraged to return to their normal, day-to-day activities as soon as possible.
Surgical Outcomes
Recently, several reports have been published on the results of vertebral augmentation procedures. These reports have raised questions about how much pain relief can be expected after kyphoplasty or vertebroplasty. Although these few studies have sparked some debate in the medical community, it is important to remember that many studies have also shown very good improvement in back pain for vertebral compression fractures.
Your surgeon will discuss realistic expectations for recovery if vertebroplasty or kyphoplasty is recommended for you.